Understanding the Menstrual Cycle: Phases, Hormones and Health
This work has been verified by our teacher: 5.02.2026 at 18:07
Homework type: Essay
Added: 3.02.2026 at 12:01
Summary:
Explore the menstrual cycle phases, key hormones, and their impact on health to deepen your biology knowledge and excel in your secondary school essay.
Biology Essay: The Menstrual Cycle
The menstrual cycle is a central aspect of human biology, shaping not only female reproductive capacity but also wider understandings of health, development, and social experience. In its essence, the menstrual cycle refers to the recurring series of hormonal and physiological changes that prepare a woman’s body for the possibility of pregnancy each month. Appreciated properly, it goes far beyond the simple notion of monthly bleeding, encompassing a delicate interplay of hormones, organs, and feedback mechanisms. In this essay, I will explore the anatomy and hormones underpinning the cycle, describe its four main phases, examine the consequences of hormonal interactions, and discuss its broader relevance to health, reproduction, and society. In doing so, the significance of the menstrual cycle – both biological and cultural – will be thoroughly brought to light.
---
Biological Foundations of the Menstrual Cycle
Anatomical Overview
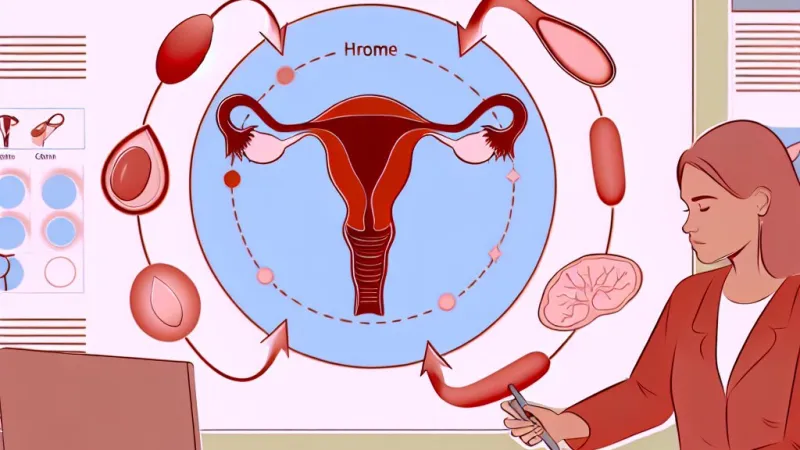
The menstrual cycle is orchestrated by several reproductive organs. The ovaries are central: small, almond-shaped structures situated on either side of the uterus, they house the eggs (ova) a female possesses from birth and generate key hormones essential for the cycle's progression. Each month, one of these eggs matures and may be released for potential fertilisation.The fallopian tubes act as passageways through which an ovum travels from the ovary to the uterus. The uterus itself, a muscular organ, has an inner lining called the endometrium which thickens in anticipation of pregnancy; here, a fertilised embryo would implant and develop. The vagina serves as the lower passage, through which menstrual blood exits the body. Together, these organs play distinct and crucial roles in both the cyclical nature of menstruation and the potential for conception.
Hormonal Regulation
Orchestration comes in the form of hormonal signals, predominantly involving four main hormones. Oestrogen helps stimulate growth and maintenance of the endometrial lining, whilst progesterone stabilises this lining and maintains it should pregnancy occur. Follicle-stimulating hormone (FSH), released by the pituitary gland in the brain, prompts eggs in the ovary to begin maturing. Luteinising hormone (LH), also from the pituitary, triggers ovulation – the moment when a mature egg is released.Notably, the hypothalamus, a part of the brain, releases a hormone called GnRH (gonadotrophin-releasing hormone) to prompt the pituitary’s FSH and LH output. This showcases the integrated communication between the brain and reproductive organs that keeps the cycle on track.
Cycle Length and Health
A typical menstrual cycle lasts around 28 days — yet a range from 21 to 35 days is considered medically normal, and many women experience natural variation over their lifetime. The regularity (or irregularity) of the cycle often acts as a window into reproductive health. Severe changes or unpredictability may signal underlying health conditions such as thyroid disorders or polycystic ovary syndrome (PCOS).---
The Phases of the Menstrual Cycle
1. Menstrual Phase (Days 1–5)
This phase marks the observable start of the cycle by the first day of bleeding. The uterus sheds its endometrial lining, which exits the body via the vagina, resulting from falling progesterone and oestrogen levels following the previous cycle’s lack of fertilisation. This process, averaging four to five days, involves uterine contractions that help expel the tissue, often causing abdominal discomfort known as cramps.2. Follicular Phase (Days 1–Ovulation)
The menstrual phase coincides with or is succeeded by the follicular phase. Here, the pituitary gland releases FSH, prompting several ovarian follicles to begin developing, although usually just one becomes dominant. Under the influence of rising oestrogen, the endometrium in the uterus proliferates – preparing for the nourishing environment needed should pregnancy occur. This phase varies more in length than others, typically lasting from day 1 to day 14 in a textbook cycle.3. Ovulation (Around Day 14)
The crescendo of hormone signalling arrives mid-cycle, when sharply rising oestrogen levels trigger a surge of LH. This LH surge leads to the rupture of the dominant follicle, releasing its mature egg into the fallopian tube – the event known as ovulation. Some women notice subtle changes at this time, such as clearer, more elastic cervical mucus or a tiny rise in their resting body temperature, both of which can help in identifying the fertile window.4. Luteal Phase (Post-ovulation to Cycle End)
After ovulation, the ruptured follicle transforms into a temporary hormone-producing structure called the corpus luteum. The corpus luteum predominantly releases progesterone, along with some oestrogen, to further prepare and sustain the now-thickened endometrium in anticipation of implantation by a fertilised egg. If fertilisation and implantation do not occur, the corpus luteum degrades, progesterone levels plummet, and the cycle recommences with menstruation.---
Hormonal Interactions and Feedback Mechanisms
The menstrual cycle is a superb example of biological regulation through feedback systems. Oestrogen, for instance, exerts different effects according to its concentration: initially, it inhibits FSH production (negative feedback), ensuring just one follicle develops to maturity; as it peaks before ovulation, it switches to a positive feedback loop, inducing the LH surge necessary for ovulation.Progesterone, in turn, suppresses both FSH and LH to prevent the development of more follicles mid-cycle. Disruptions to these interactions—such as by illness, excessive stress, or conditions like PCOS—can result in irregular cycles or even amenorrhoea (absence of periods), highlighting the importance of hormonal balance for reproductive health.
---
Physiological and Psychological Effects
Throughout the cycle, individuals can experience a variety of physical symptoms. The menstrual phase is infamous for discomfort, including lower abdominal pain (dysmenorrhoea), bloating, tender breasts, headaches, and general fatigue. Some women also experience *mittelschmerz* (German for "middle pain"), a sharp twinge felt during ovulation as the follicle releases the egg.Apart from bodily symptoms, the cycle’s impact on mood and mental functioning should not be underestimated. Hormonal fluctuations – notably, oestrogen’s influence on serotonin, a brain chemical associated with wellbeing – can cause mood swings, irritability, or low mood. Concentration and memory might feel subtly affected at various phases. However, not every person experiences these changes to the same degree; diversity in cycle symptoms is entirely normal.
Monitoring one's cycle, either through modern apps or traditional methods like temperature charting, is becoming popular. This self-knowledge can help individuals spot unusual patterns which may indicate underlying health issues and utilise periods of fertility to either pursue or avoid pregnancy according to their wishes.
---
The Menstrual Cycle and Reproduction
Biologically, the menstrual cycle’s organisation dramatically increases the chances of successful fertilisation and pregnancy. Ovulation, the point of egg release, represents the most fertile period of the cycle – and timing intercourse accordingly is at the heart of ‘natural family planning’ methods.A healthy endometrium, sustained by balanced hormone production, is vital for the implantation of a fertilised egg. The absence of menstruation (amenorrhoea) beyond the expected time is often an early sign of pregnancy. Conversely, external factors such as significant stress, changes in body weight, or chronic illnesses (like diabetes) can disrupt regular cycles, affecting fertility in the process.
From a clinical perspective, the cycle can be modified or interrupted by hormonal contraceptives, which mimic pregnancy-like hormone levels to prevent ovulation. Assisted reproductive technologies (ART), such as IVF, rely on an in-depth understanding of the cycle to optimise timing and success rates.
---
Cultural and Social Perspectives
In Britain and elsewhere, the menstrual cycle has been the subject of long-standing cultural taboos and misunderstandings. Literature, such as Virginia Woolf’s *To the Lighthouse*, subtly references the burdens of unspoken female experiences, including menstruation. In the past, myths around “uncleanliness” or incapacity during menstruation have permeated social thinking, sometimes leading to embarrassment or even discrimination.However, there has been marked progress in public awareness and acceptance, particularly in recent times. Schools now include comprehensive sex and relationships education (RSHE) in their curriculum, with particular focus on menstrual health – as per Department for Education guidelines. Campaigns to increase access to menstrual products for schoolgirls—reflecting concerns over “period poverty”—have gained traction, recognising that lack of resources can impact education and self-esteem.
Other UK initiatives, such as Scotland’s world-leading decision to provide free period products in public buildings, exemplify a societal shift towards destigmatisation and support. Menstrual wellbeing campaigns, like those run by the charity Bloody Good Period, evidence a growing recognition of menstruation as a public health and equality issue rather than simply an individual problem.
---
Rate:
Log in to rate the work.
Log in